Air Ocean Maroc provides comprehensive aviation services, so the complex case of a transpulmonary ultrasound was well within their remit. It’s a prime example of exceptional teamwork under pressure.
Transpulmonary ultrasound allows a quick and non-invasive evaluation of lung function and the presence of potentially serious pathologies during flight. In case of a medical emergency onboard a plane, transpulmonary ultrasound can quickly evaluate the severity of a condition, leading to appropriate decisions. It also detects lung pathologies that can be worsened by changes in atmospheric pressure.
As we know, altitude impacts the respiratory system, due to the decrease in atmospheric pressure and oxygen concentration. This leads to disorders such as hypoxia (decrease in tissue oxygenation), hyperventilation (increase in frequency and depth of breathing) and accumulation of carbon dioxide in the blood (hypercapnia). Pneumothorax is when air leaks into the pleural cavity (space between lungs and chest wall) and compresses the lung, causing difficulty breathing and chest pain. Those with respiratory failure are at greater risk of pneumothorax, as the lung is damaged or diseased. This risk increases during flights, as air pressure can vary significantly. Also, people with respiratory failure are more sensitive to changes in atmospheric pressure.
African evacuation
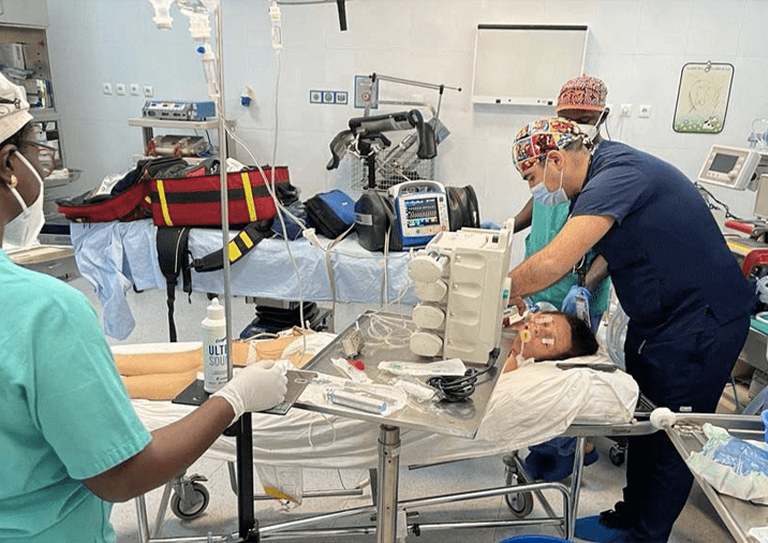
We recently evacuated a patient from a landlocked country in Africa, who had a hypoxic lung infection for which she was intubated and put on mechanical ventilation. Lacking resuscitation services, she was kept under an anesthesia ventilator in the operating theatre until the arrival of the Air Ocean Maroc medical team (knowing the risk of barotrauma with this kind of ventilator).
The patient was haemodynamically stable, saturation was 97 per cent under 70 per cent oxygen, with plateau pressure after connection to our ventilator at 26 due to a lack of radiological exploration within the structure. A transpulmonary ultrasound visualised the absence of pleural sliding on the superolateral quadrant of the right lung. The decision was to board the patient head forward of the plane to have access to the right lung, in case of worsening pneumothorax.
Our medical team performed ultrasound examinations closely at altitude, noticing the increase in peak and plateau pressures, with increased oxygen requirements and thoracic asymmetry. On transpulmonary ultrasound, there was disappearance of pleural sliding over more than three right lung quadrants, indicating a drainage was required, and it was the only way to save the patient.
Carried out by an experienced team, the drain connected via a jar filled with serum on aspiration. The bubbling was a sign of success, as well as the improvement of the patient’s respiratory condition. The control of the drainage was carried out using ultrasound, which visualised the resumption of sliding in all thoracic quadrants. Our patient arrived safely at her destination and was received by a well-equipped ground medical team, who had been informed of developments by satellite calls.
Quick evaluation
In terms of air ambulance, transpulmonary ultrasound plays a very important role in the diagnostic orientation of respiratory failures, particularly in regions where access to medical care is limited. With respiratory distress, transpulmonary ultrasound can help doctors quickly evaluate the condition and make appropriate therapeutic decisions, such as performing a thoracostomy or placing a pleural drainage catheter. It thus allows for a more efficient repatriation of patients requiring specific care.
It is important to note that transpulmonary ultrasound should be performed by a doctor trained in this technique – and cannot replace radiologic exams for all indications. However, it is considered a useful tool for evaluating patients in an aerospace emergency, or during air ambulance evacuation in regions where access to medical care is limited and radiologic equipment is lacking.






No comments for “Case study: Air Ocean Maroc on the the complex case of a transpulmonary ultrasound”